Fertility is a human right, as well as being one of the functions of life for all living organisations. If you want to have a baby but can’t conceive naturally then you must seek help from a fertility specialist. Infertility is a disease of the reproductive system defined by the failure to achieve pregnancy after 12 months of unprotected sex. If the female age is over 35, then help should be sought after only 6 months.
As part of the diagnostic process for this disease, following consultation of your medical and sexual history, certain tests are required.
But which ones do you need?
It’s worth bearing in mind that infertility is a two-way street. It is not just women who need to be tested. Male factor accounts for 20-30% of all cases where couples fail to conceive. 20-30% of cases is attributable to where both partners. All established tests are always useful, so it is probably more helpful to group them into the categories of need to have and nice to have.
Need to have
Women
Blood tests: samples of blood can be tested for progesterone to check on ovulating status. The timing of this test is based on how regular the patient’s periods are.
- If a woman has irregular periods, she’ll usually be offered a blood test to measure hormones called gonadotrophins, which stimulate the ovaries to produce eggs
- A blood test for Anti Mullerian Hormone (AMH) is an important indicator for ovarian reserve (the number of available eggs). This is especially important for women over 35 whose egg numbers have decreased and where egg quality may also decline.
Hysterosalpingogram (HSG): this is an X-Ray to determine whether fallopian tubes are blocked or damaged. The fallopian tubes connect the ovaries to the uterus and the egg must pass through them in order for pregnancy to occur. As well as blockages, fallopian tubes can be scarred, sometimes called adhesions as a result of previous infections, surgery or endometriosis.

Ultrasound: this uses high frequency sound waves to image the ovaries and uterus to check for abnormalities that could prevent pregnancy.
Men
Semen sample: the semen is tested for the quality and quantity of sperm. General health parameters of sperm include the number of cells, the ability to swim, volume of liquid, vitality and pH (a measure of acidity/alkalinity).
Nice to have
These are tests that may not be routine, but which a health care professional may consider to be useful in a particular case. They are nice to have but not as essential as the need to have ones listed above.
Women

Chlamydia test: Chlamydia is a sexually transmitted infection (STI) that can affect fertility. A swab, similar to a cotton bud, but smaller, soft and rounded is used to collect some cells from the cervix to test for chlamydia. However, a urine test may be used as an alternative. A positive result will require antibiotic treatment.
Cervical mucus test: cervical mucus test helps health care professionals to see if there are any antagonistic antibodies in there that might be killing the sperm. The mucus also should be of the ideal consistency (raw egg white appearance) to create a sperm-friendly environment.
Men
Chlamydia test: since chlamydia is an STI, it is likely that both partners in a male/female relationship will have it if one partner tests positive. But anyone who is sexually active is at risk. For men, a urine sample is taken to test for the infection.
Sperm penetration test: this is another advanced male infertility test. It evaluates the ability of the sperm to penetrate the cervical mucous, which is central to conception.
Acrosome reaction test: this test is designed to evaluate sperm performance; in particular how well a sperm is able to perform during the fertilisation process.
Advanced tests
These are tests that follow on from the need to have tests above and only if a health care professionals decides they are necessary.
They can include:
- Laparoscopy (women): this is a form of keyhole surgery, which involves making a small cut in the abdomen so a thin tube with a camera at the end (a laparoscope) can be inserted to examine the uterus, fallopian tubes and ovaries.
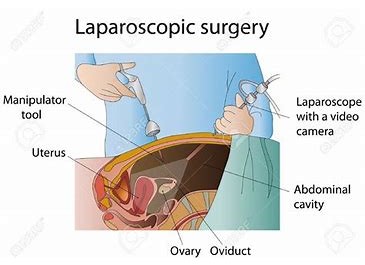
- Dye may be injected into the fallopian tubes through the cervix to highlight any blockages in them
- Laparoscopy is usually only performed if it’s likely that there may be a problem. For example, if a patient has had an episode of pelvic inflammatory disease (PID) in the past, or if ultrasound suggests a possible blockage in the tubes.
Hysteroscopy (women): this uses a small camera that is inserted into the uterus through the vagina to check for any fibroid or polyp growth or any kind of scarring.
Endometrial biopsy (women): in this test a small piece of the uterine lining is taken and examined under a powerful microscope to check for signs of its proper development and to see how it responds to the hormone progesterone. It is usually done between Day 18 and 28 of the cycle.
Magnetic resonance imaging (MRI) for either male or female: this is a more expensive test that can provide useful information about the uterine wall in women, and about the testes in men. For women it can be helpful in cases of endometriosis, as well as pelvic cysts, IVF failures, and painful periods.
Routine tests prior to treatment
This is not an exhaustive list by any means, but just covers the MAIN types of test that a fertility patient might encounter before undergoing any treatment. For instance, in many parts of the world it is routine to also test for infections before any treatment is undertaken such as HIV, Hepatitis, Rubella, although these tests are not indicative of fertility.
When patients are actually in cycle other specialised tests are undertaken to ensure that everything is progressing to plan. These determine the optimal treatment and the timing. For example, folliculometry tracks the events of a growing follicle through a regular menstrual cycle from day 9 to day 20 with repeated scans.
As always, every case is unique in its own way, and therefore the best advice on the tests you might need will come from your healthcare provider.


